Eczema, also known as atopic dermatitis, is not caused by a specific bacterium. Instead, it is a complex condition that involves genetic, environmental, and immunological factors. Skin infections are common in people with eczema, and it is highly likely that you will develop a bacterial, fungal, or viral infection at some point. All of these infections necessitate treatment in order to be eradicated.
up as they do not improve on their own. The quicker the infection is recognised and the sooner treatment is started, the better the response to treatment will be. Preventing infection is also important – from simple hand-washing before applying your creams to more sophisticated methods using antiseptics.
When you have eczema, the top layer of the skin (the epidermis) is often damaged. This damage can be visible to the naked eye, appearing as cracks and areas opened up by scratching. There is also less protection within the skin, which you cannot see. These alterations in the barrier function of the skin increase the potential for skin infection. Infections that develop because of the underlying condition of eczema are often described as ‘secondary infections’.
The exact cause of eczema is not fully understood, but it is believed to be a result of a combination of:
- Genetic factors: A family history of eczema, asthma, or allergies can increase the risk of developing the condition. Certain genetic variations may also play a role in the skin’s barrier function and immune response.
- Immune system dysfunction: Eczema is associated with an overactive immune response, which can lead to inflammation and skin irritation.
- Skin barrier dysfunction: People with eczema often have a compromised skin barrier, which allows moisture to escape and allergens or irritants to penetrate the skin, leading to dryness, itching, and inflammation.
- Environmental triggers: Various environmental factors can trigger or worsen eczema symptoms. These may include exposure to allergens like pollen, pet dander, dust mites, or irritants like harsh soaps, detergents, and chemicals.
While bacteria do not cause eczema, they can play a role in secondary infections. Scratching the itchy skin can lead to open wounds, and bacteria may colonize these areas, leading to infection. Common bacteria associated with secondary infections in eczema include Staphylococcus aureus and Streptococcus pyogenes. If a secondary infection occurs, it is important to seek medical attention for appropriate treatment.
Bacterial infections
The skin is the most important protection we have against infection as it provides a barrier that prevents the billions of bacteria found on our skin from entering the body.
Staphylococcus aureus (Staph. aureus) is the bacterium that is most commonly responsible for secondary infection of eczema. It is often associated with hair follicle infections (folliculitis), boils and abscesses. ‘Impetiginized eczema’ is another label or name given to eczema infected with Staph. aureus. When the bacteria penetrate the epidermis, an immune reaction can be triggered, which aggravates the eczema and brings about a flare.
Initially, eczema infected by Staph. aureus will appear itchy and red or darker than your usual skin colour, depending on skin tone. If you look closely in natural light, you might see a tangerine glisten to the skin – a little bit like orange body shimmer dust. As the infection progresses, weeping and crusting with a yellow/golden tinge will be evident.
Bacterial skin infections are treated with antibiotics, either topically (applied to the skin) using a cream, or orally (by mouth) in the form of tablets or a liquid suspension. Whether the doctor gives you a topical or oral treatment depends on the size of the affected area/s and number of places where the infection occurs. It is important when treating the infection with a cream that you apply it consistently and for the prescribed duration (in the same way you would take a course of oral antibiotics). Topical antibiotics should not be used for longer than 14 days due to the risk of bacterial resistance.
Skin infections can sometimes be caused by a resistant strain of Staphylococcus aureus such as methicillin-resistant Staph. aureus (MRSA), often referred to as a ‘superbug’ in the media. If you are not responding to antibiotics, a skin swab should be taken to confirm the strain of bacteria and the antibiotics to which it is sensitive. MRSA bacteria are usually spread through skin-to-skin contact with someone who has an MRSA infection or has the bacteria living on their skin. MRSA can also be spread through contact with everyday objects such as towels, sheets, taps, surfaces and door handles.
There are some steps you can take to reduce your risk of picking this up:
- Careful hand-washing before applying your emollients and treatments.
- When visiting a clinic or hospital, use the hand gels available beside doorways and report any unclean toilet or bathroom facilities to the staff.
Fortunately, MRSA bacteria are not resistant to all antibiotics, so MRSA infections can be treated. Skin infections due to MRSA are usually treated with antibiotics in tablet form, or sometimes injections if the infection is widespread.
Fungal infections
As with bacteria, certain fungi live naturally on everyone’s skin. There are two main fungal infections that infect people with eczema. One is caused by candida, a yeast that thrives in warm, moist areas of the body such as under the arm, groin, and the neck area in children. The other type originates from moulds called dermatophytes that cause an infection known as tinea or ringworm (this describes the shape of the skin lesions and has nothing to do with actual worms!).
Candida infections can be treated with a cream containing clotrimazole. This can be purchased from a pharmacy.
Tinea infections are named according to the part of the body where they are found: tinea corporis on a body site, tinea capitis on the scalp, tinea pedis on the feet. Tinea infections are often difficult to distinguish from discoid eczema. Usually the doctor or nurse will prescribe a fungal treatment (miconazole cream) – also available over the counter from a pharmacy – to see if the skin responds and the lesions clear. For tinea infections of the scalp or nails, an oral antifungal agent will be necessary. Your GP will need to prescribe this. A skin scraping can be taken for mycology (fungal) analysis when there is difficulty resolving the lesions and there is doubt about the diagnosis.
Antifungal creams do not entail the same resistance concerns as antibiotic creams, so you can apply them as and when they are needed. For best results, consistency with application is required until the lesions are clear, applying three times a day or as directed by your doctor.
Viral infections
Eczema herpeticum
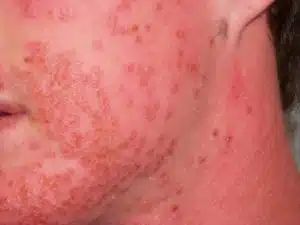
The herpes simplex virus usually just causes cold sores, but in people with eczema it can spread through the skin and develop quickly into a serious condition called eczema herpeticum. The symptoms of this viral infection include:
- areas of painful eczema that quickly get worse
- groups of fluid-filled blisters that break open and leave small, shallow, open sores on the skin
- a high temperature and generally feeling unwell (in some cases).
Obtaining treatment quickly is important with this infection – it should not be left until morning! You should see a doctor immediately if you think you have eczema herpeticum; and if you cannot be seen by your GP, call NHS 111 or attend the nearest A&E department.
The virus is spread through direct contact, both skin to skin and contact with surfaces (the virus can live for a few hours on a hard surface). To prevent infection spreading, let the surgery or hospital staff know on arrival that you think you have eczema herpeticum, so you can wait in a private area until the doctor assesses you. If you have eczema herpeticum, you will be treated with an antiviral drug called aciclovir; often patients are admitted to hospital for a few days in order to receive the therapy intravenously.
Common childhood infections and infestations
Childhood infections, which can be worse when you have an underlying diagnosis of eczema, include the following:
Chickenpox
The presentation of chickenpox can be variable, from just a few pustules to extensive pustules covering the entire skin’s surface and inside the mouth and ears. The infection is spread through blood, saliva and cough droplets.
Children with atopic eczema have a slightly higher likelihood of developing a complication of the infection. Parents will need to closely monitor them and their well-being by checking their temperature, looking for infected lesions and seeking medical advice if concerned.
If you have taken oral steroids within three months of contracting chickenpox, you may have a lowered ability to fight the infection and you will require closer monitoring by your GP. Oral antivirals or hospital admission may be needed to prevent complications. Topical steroids and topical calcineurin inhibitors (pimecrolimus and tacrolimus) are less of an issue. See your GP for advice on continuing these treatments while you have new chickenpox lesions. Calamine lotion can be drying on the skin and is not usually helpful in children with eczema.
Molluscum contagiosum
This is a common childhood infection. The papules last between a few months and up to two years. They are highly contagious, and rubbing or scratching them helps them to spread on the skin. Treatment is not usually given as these viral lesions do eventually go away by themselves.
Scabies
Scabies are tiny mites that burrow and lay eggs in the outer layers of skin. Scabies infestations are very itchy and produce a rash. They are more common in children with eczema and are difficult to diagnose as the presentation is similar to that of eczema; also, the scabies may be hidden by the eczema. Scabies like warm places, such as skin folds, webs of the fingers, the feet and around the buttock or breast creases. They can also hide under watch straps, bracelets or rings. The incubation period is up to 8 weeks, and dry, scratched skin helps the infestation to spread. See your GP or pharmacist if you think you have scabies – it is not a serious condition but it does need treating. Permethrin cream and malathion lotion are medications that contain insecticides that kill the scabies mite. They are available to purchase over the counter from a pharmacist.
Preventing infection
Simple measures to help prevent infection include the following:
- Always wash your hands before applying topical treatments.
- Remember to decant emollients from any tubs you may be using – if you dip your fingers into a tub, it can easily become contaminated with bacteria. A metal dessert spoon is good for decanting emollient and washes well under the tap. If you are using pump handle dispensers for your emollients, you do not need to decant – you can just pump the emollient onto your hand (avoid touching the nozzle).
- If your eczema is infected by Staph. aureus, or you have a fungal or viral infection, avoid sharing towels, bedding and clothing until the infection has cleared.
- Some people with eczema suffer recurrent bacterial infections and require antibiotic treatment on several occasions. These people are often advised to use antiseptic washes or creams to reduce the amount of Staph. aureus on the skin. Commonly these antiseptics are triclosan, chlorhexidine gluconate or sodium hypochlorite. These antiseptics come combined with emollient preparations and can be used to wash with in the bath or shower, or applied as a leave-on preparation. One of the advantages of controlling infections with antiseptics is that they do not create bacterial resistance.
- Bleach bathing is a treatment option for people who experience recurrent infections. Bleach bathing uses the chemical sodium hypochlorite, which is effective against bacteria, fungi, viruses and MRSA. The principle of bleach bathing is to bathe in the bleach solution twice a week, and continue with your usual treatment routine in between.
A review of the research available on bleach bathing (Cochrane systematic review, published in October 2019), found that bleach baths were unlikely to make any difference to eczema or to patients’ quality of life. If you try bleach bathing, do so with caution and discuss it with your doctor first. Care must be taken as the wrong substance or too high a concentration can be harmful.
You must not use household bleach for bleach bathing as the concentration of sodium hypochlorite will vary in products and most will have additional chemicals that could damage your skin.
Milton Sterilising Fluid, at a strength of 2% sodium hypochlorite, is the only product that currently provides the strength used in research trials. It has been adopted by hospitals and can be bought cheaply from pharmacies. It does not contain any perfumes or colourants and does not degrade, so it provides a stable strength.
The following instructions are for a standard full-size bath:
- Fill the bath with warm water to around 10cm depth. This is usually around 60 litres. You can use a measuring jug or bucket the first time to help work out how much this looks like. Make a mark on the bath tub for future filling – a small strip of Gaffer tape just above the water line works well for this.
- Add 125ml or 1/2 a cup of Milton Sterilising Fluid to the water and completely mix it in (around 2ml per litre of bathwater).
- Soak in the bath water up to your neck for ten minutes. For smaller children, you can use a sponge or flannel to soak any dry and affected areas that are out of the water.
- Do not splash water onto the face as it will irritate the eyes.
- Rinse yourself or your child well with fresh warm water, for example, in the shower.
- Pat the skin gently dry with a soft towel and apply emollient.
It’s important to note that eczema is not contagious, and you cannot “catch” it from someone else. If you or someone you know is experiencing symptoms of eczema, it’s best to consult a healthcare professional or a dermatologist for an accurate diagnosis and appropriate management.